Stress definitely leads to anxiety, just as isolation gives way to depression.
Psychological and social experiences shape the brain and can potentially lead to mental health problems, but the underlying mechanisms – how these experiences translate into physiological changes in the brain – remain poorly understood.
Now psychological scientists may have found a missing link.
“We actually have biomarkers that really show links between psychological processes and people’s physiology,” says Christopher Fagundes, a professor of psychological sciences at Rice University.
In a review published in Current directions in psychological science, Fagundes and his colleagues argue that the missing link may be the mitochondria, the power plant of the school cell.
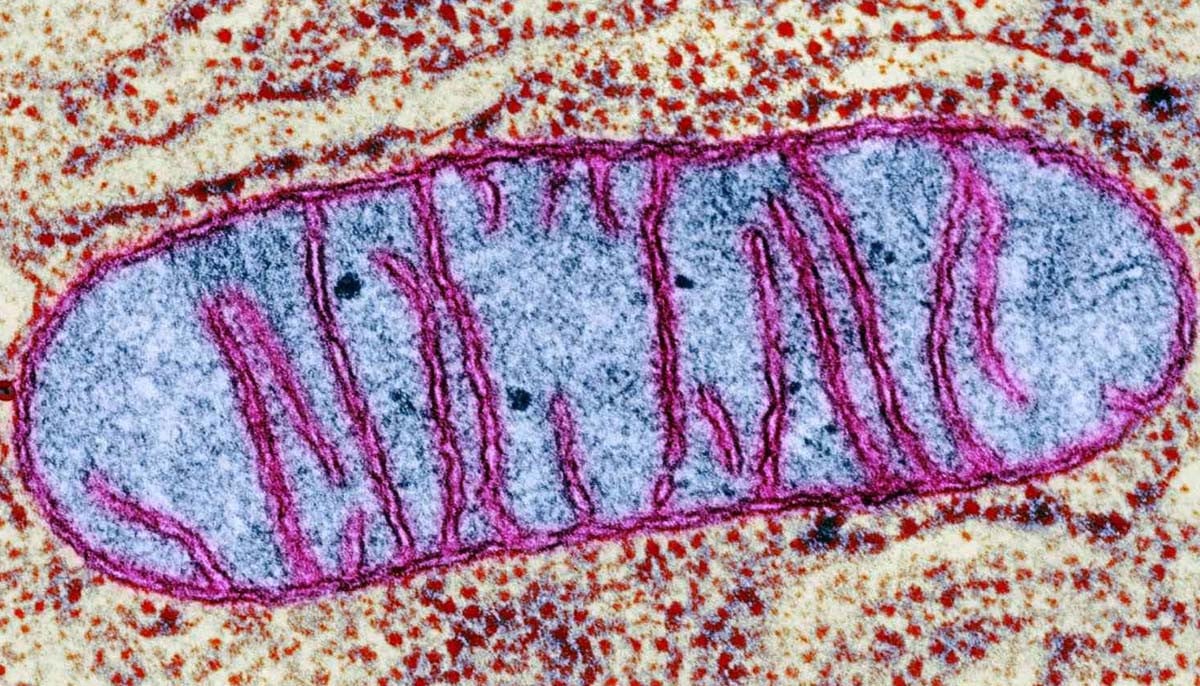
Mitochondria are best known as the bean-shaped cell organelles that play a crucial role in generating energy.
But they are now recognized for many more roles, including their role in immune signaling, stress responses and neural functioning.
They are sensitive to changes in environmental and social conditions, suggesting that stress, loneliness and trauma can target mitochondria, leading to downstream psychological effects. Changes in mitochondrial function have been linked to anxiety, depression, post-traumatic stress disorder (PTSD), Alzheimer’s disease and other neurological disorders, as well as physical health consequences such as cardiovascular disease, diabetes and certain cancers.
“The actual cellular machinery that links these experiences to disease actually starts at the level of the mitochondria,” Fagundes said in an interview with the Observer.
“Everything we think about in terms of oxidative stress, to the fatigue we feel, to the byproducts that arise when stressors get out of control, it really underlies that,” he added.
The high energy demands of the brain make it particularly vulnerable to mitochondrial dysfunction. When mitochondria are less efficient, there is less energy for neurotransmission (transmission of brain signals), affecting processes that support mood regulation and memory.
“A lot of the relationships we’ve been thinking about-[between] inflammatory processes and these types of mental health outcomes – we need to look at changes in mitochondria could be a real mediator [underlying] mechanism,” Fagundes said.
To date, few studies have examined the effects of improving social support on mitochondrial function. More research into these and other ways to improve mitochondrial resilience – and the different roles mitochondria play in the brain – could be key to better understanding and developing better treatments for a variety of mental and physical disorders.
“We’ve talked a lot about things like inflammation. It tells us that something is happening, but mitochondria help us explain why it’s happening at the cellular level,” Fagundes said before concluding: “If we focus more on the cellular level, we will gain a much deeper understanding of the underlying processes.”